The federal health insurance exchanges launched in 2013 to a modestly encouraging but tepid insurer response. Anxious at the prospect of developing consumer insurance products to be sold through a relatively untested channel and targeted at a challenging demographic, many large insurers adopted a wait and see approach. While the marketplaces exceeded enrollment targets and enabled millions of Americans to purchase insurance, consumers in many markets faced limited options. In several states, such as New Hampshire, Mississippi, and Rhode Island, only one or two insurers participated on the exchanges.
Core to the public insurance marketplace thesis was the concept that a larger individual insurance market would attract competition, which would in turn reduce prices. However, many in the industry understood that competition on the exchange would not mature overnight. Prior to the Affordable Care Act, it was not uncommon for the dominant player in a state’s individual insurance market to enjoy a 50% market share. As coverage year 2015 health exchange filings become available, we can start to examine the relationship between market competition and insurance premiums on the federal exchange.
My first analytical approach was to plot the mean monthly premium in each state (by coverage level) against the number of unique insurers in each market (see R code on Github). A basic linear regression of premiums by number of unique insurers and by coverage level revealed no significant relationship.
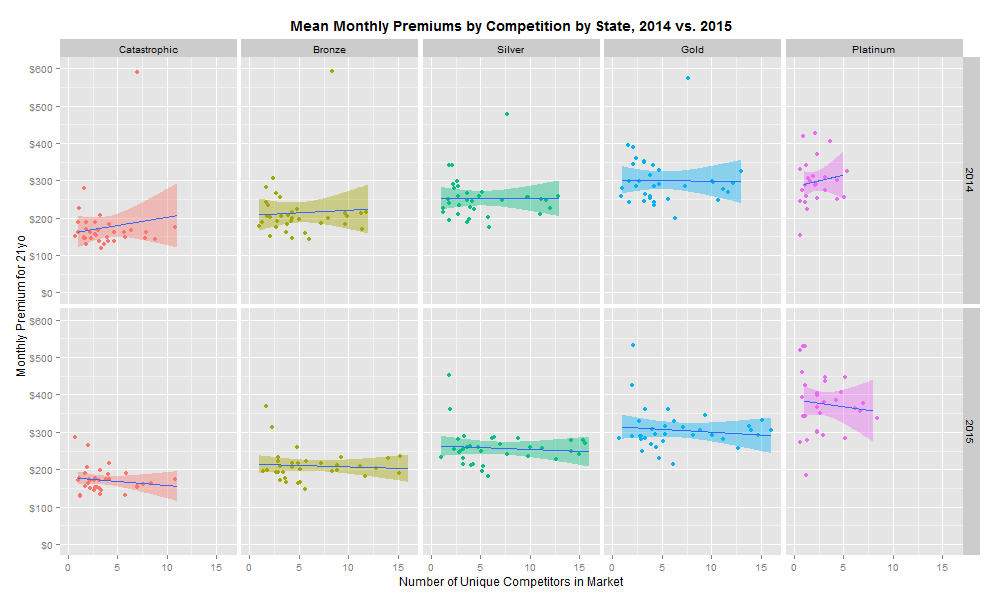
This is clearly a disappointing discovery. However, it is possible that the important unit of analysis is not the mean premium in each market, but instead the minimum premium in each market. Repeating the same analysis with the lowest premium as our dependent variable reveals the following:
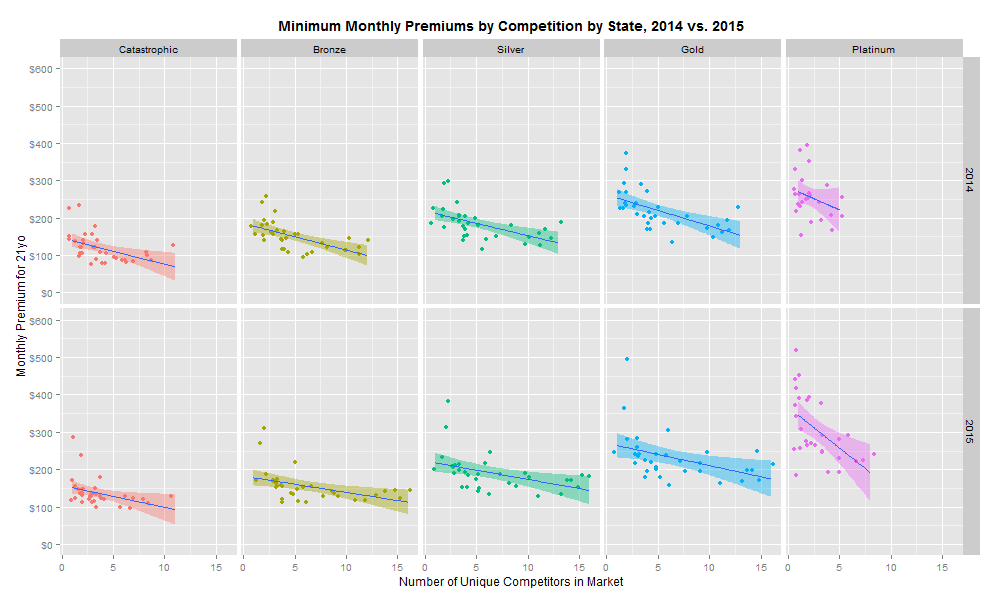
There is a significant negative relationship between increased competition and health insurance premiums for all coverage levels in 2014 and 2015. The regression model (collapsing 2014 and 2015 rates) suggests that each incremental market entrant corresponds to a 3.4% reduction in monthly premiums. Moreover, this trend continued as more entrants entered the market in 2015. However, linear regressions by year suggest that the size of the competition relationship is decreasing: the effect of an incremental insurer on premiums was -3.7% in 2014 and -3.1% in 2015.
A variety of potential factors could explain this pattern:
- As more insurers enter a market, the relatively fixed population is fragmented across a larger number of discrete risk pools, which leads to greater actuarial risk. However, an insurer with a dominant market share or national footprint may pool primary or secondary risk. A reduced risk profile should lead to lower premiums.
- In some markets, the past decade of provider consolidation afforded integrated delivery systems and academic medical centers with more negotiating leverage, which has led to higher contract rates. This may pose a particular challenge to new or young insurers (10-15% of the exchange market) that lack the patient volume to obtain the deep discounts required to compete on price.
- Selling insurance directly to consumers contributes to substantially higher marketing and administrative costs. However, national carriers may benefit from some scale efficiencies. Larger markets likely attract more insurers, and national insurers with potentially lower administrative costs are more likely to participate in these markets.
- Medical Loss Ratio (MLR) requirements squeeze all insurers into a narrow margin band, which deters all but the most confident and price competitive entrants. A failure to reduce mean premiums might imply that insurers are approaching a theoretical local maximum on profitability. Low margins, even on high top-line revenue, might impinge insurers’ abilities to invest in innovative benefit designs and reimbursement structures to dramatically improve savings.
These are some plausible factors that may contribute to the observed patterns, and it is important to not read too closely into such a simple analysis. The key challenge behind this dynamic is that the nature of price competition is still predominantly volume-based and not value-based. In other words, insurers in this market reduce costs by leveraging the number of patient lives they have to obtain discounts from providers, and not by fundamentally changing the incentive structures to reward cost effective improvements in patient outcomes. Only through the proper alignment of reimbursement with outcomes will our system be able to drive the transformative reduction in total costs and improvements in patient care.